Working to end mental health stigma in BIPOC communities
July is Black, Indigenous, People of Color (BIPOC) Mental Health Month, an initiative developed by Mental Health America to increase public awareness of mental illness, especially among BIPOC communit
Key takeaways
July is Black, Indigenous, People of Color (BIPOC) Mental Health Month, an initiative developed by Mental Health America to increase public awareness of mental illness, especially among BIPOC communities. Especially now, we must recognize that marginalized, oppressed, and disenfranchised persons experience unique concerns, traumas, stress, obstacles, and challenges due to historical experiences, cultural differences, and social issues. Unfortunately, there are many barriers that people of color face when seeking mental health treatment that must be addressed.
Mental health in BIPOC communities
BIPOC communities face several challenges when it comes to mental health conditions and seeking care. In general, BIPOC individuals don't seek treatment as frequently as whites for mental health issues. According to the American Psychiatric Association, “In 2015, among adults with any mental illness, 48% of whites received mental health services, compared with 31% of Blacks and Hispanics, and 22% of Asians.”
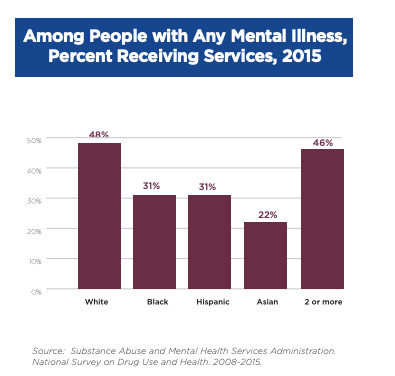
Barriers to seeking treatment
There are several barriers that keep those in BIPOC communities from seeking mental health treatment, including:
- Language and culture differences
- Socioeconomic disparities
- Stigma and fear
- Legal or immigration status
- Provider bias and cultural incompetence
Each of these factors presents its own unique set of challenges, but the most common barrier—and perhaps the most difficult to overcome—is the prevalence of stigma surrounding mental health in BIPOC communities.
The role of stigma
BIPOC communities experience higher stigmatization of mental health conditions and treatment than the general population due to the common narrative in BIPOC communities that mental health is a weakness. Due to this stigma, open conversation about mental health and personal or family issues affecting mental health is discouraged or disregarded. According to Mental Health America, “Research indicates that Blacks and African Americans believe that mild depression or anxiety would be considered “crazy” in their social circles. Furthermore, many believe that discussions about mental illness would not be appropriate even among families.”
Often, individuals of color do not see therapy or mental health services as an option because of these cultural pressures. If they wish to pursue mental health treatment, individuals in BIPOC communities are forced to break through the shame, fear, discomfort, and vulnerability often associated with mental health care. For groups already subjected to discrimination, stigma only further hinders their ability to seek mental health treatment. In addition to racial and cultural stigmas, there are also self-stigmas that individuals place on themselves surrounding the idea of mental health issues. There’s a belief that if you need medication or therapy, you are crazy; however, this negative association doesn’t just come from society but frequently stems from an internal monologue.
Addressing the problem
With less than 30% of licensed professional counselors in the U.S. being part of the BIPOC community, these disparities are deeply rooted in the profession and ultimately affect the accessibility of mental health care. This lack of BIPOC providers presents yet another barrier to people of color seeking mental health treatment. Communities of color require culturally competent mental health providers who demonstrate cultural sensitivity and use appropriate language and communication patterns to make their patients as comfortable as possible.
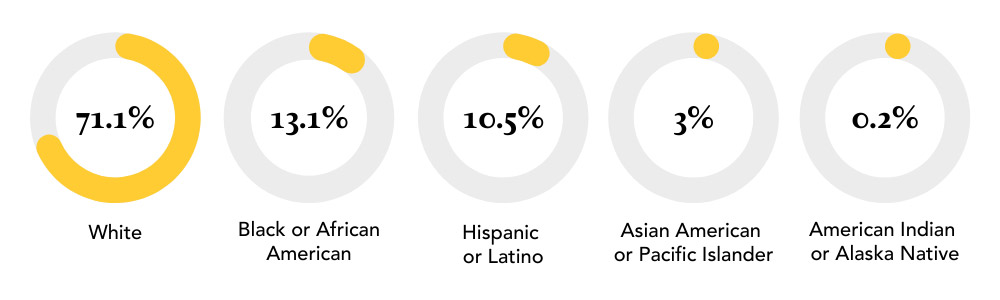
Today, all health care providers should be trained to serve multi-ethnic consumers. According to counseling.org, “It is vital to have culturally competent professional counselors provide a safe and trusting environment and assist in eradicating minority stigma, bias, and mental health misdiagnosis.” By increasing the cultural diversity within the mental health professions, BIPOC individuals will have the ability to establish stronger, trusting relationships and break through the barriers that inhibit them from seeking mental health care.
To work towards more open, inclusive conversations, there need to be significant changes to how we talk about and treat BIPOC mental health issues. Raising awareness of the barriers BIPOC communities face to receiving quality mental health care is only the first step in achieving mental health equity. In addition to bringing awareness to these issues during BIPOC Mental Health Month, it's important to work toward improving access to mental health care for people of color year-round.
BIPOC mental health at Talkiatry
At Talkiatry, we believe that in all communities, mental health care should be as accepted as physical health care. In addition, mental illness should not be stigmatized or feared, as it is a real condition that can be diagnosed and treated. We aim to do our part to combat disparities and stigmas in mental health care, and to foster trust between BIPOC communities and mental health providers.
Talkiatry provides outpatient mental healthcare services including diagnosis, psychotherapy, and medication management to people from all communities. As our practice grows, we are dedicated to building a team of mental health providers from richly diverse backgrounds, creating a safe and welcoming environment for people of color to seek psychiatric treatment with culturally sensitive practitioners.
We are committed to providing you with accessible and affordable in-network mental health care solutions. We provide customized treatment plans focused on helping you feel better, faster. We also offer flexible telemedicine and in-office appointment options to match our therapeutic and modern approach to psychiatric care.
Talkiatry is a mental health practice, and our clinicians review everything we write. However, articles are never a substitute for professional medical advice, diagnosis, or treatment. If you think you may need mental health help, talk to a psychiatrist. If you or someone you know may be in danger, call 911 or the National Suicide and Crisis Lifeline at 988 right away.






